The US faces an HPV epidemic, yet there is still little known about the virus. A Florida-based grassroots organization, HPV Awakening, is fighting to expand research about the virus to provide resources for treatment and prevention. Public awareness is in desperate need of an energy boost.

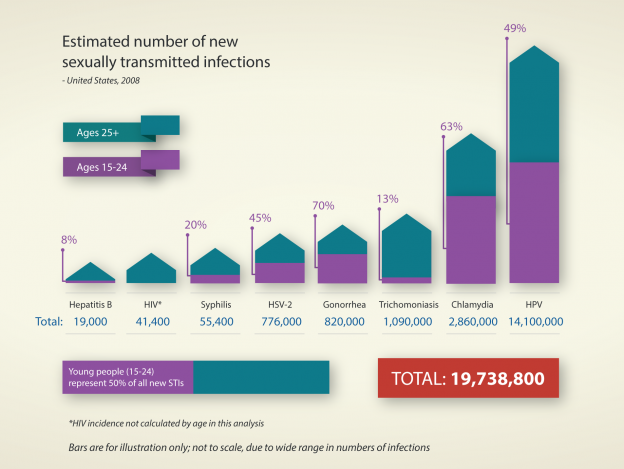
HPV is the most prevalent and rapidly spreading STI in the USA according to a February 2013 report (PDF) by the CDC (Center for Disease Control and Prevention). Based on the most recent data on STIs in 2008, the report finds approximately 80 million Americans are infected with some form of HPV- which makes up 71% of all STI infections in the country. And it is spreading fast, as most people with HPV do not know they are infected. Fourteen million will become newly infected this year. This means that almost every sexually active person in the US (regardless of sexual orientation, number of partners, age, income, etc.) will acquire HPV at some point in their lives. In other words, we are officially in an HPV crisis.
Sounds pretty serious, eh? In most cases, HPV will go away by itself before it causes any health problems- particularly in young people. The problem is that there are many variations and strains of HPV- 40 of which are related to cancer- and there remains much unknown medically about the virus and how to detect it.
For example, there is no certain way to tell who will develop health problems from HPV and who will not. For men, there is currently no FDA-approved HPV test, which means that men who have clear STI screenings with negative results should not consider themselves HPV-free or at zero-risk. The only form of testing a male can have is through an anal pap smear (used to check for anal cancer), and only if he has been the recipient of anal sex, not directly as a method to check for HPV. For women, there are test to directly detect the virus, but they are not mandatory- you still have to specifically ask for them, despite how prevalent HPV is in the USA. In 2009, the FDA approved DNA testing for HPV yet blood donations and samples are not screened.
What is HPV? Human Papillomavirus is an infection of the skin and mucous membranes. There are over 100 strains of HPV of which 40 are identified as sexually transmitted infections. It is often called “genital warts”, because when a strain causes warts (not all do) and symptoms are visible it appears as tiny cauliflower-like clusters on the genitals. These HPV types can also infect the mouth and throat. Other strains are cancerous and some are a direct cause of cervical, anal, and oral cancer. On average, about 15,000 women get diagnosed yearly with cervical cancer and about 80% of these cases are cause by HPV.
In most cases, HPV shows no symptoms yet remains highly contagious, and unfortunately, condoms do not offer 100% protection. However, they are by far safer than going without protection. It is generally stated by health organizations that condoms provide approximately 70% protection against HPV.
How does it spread? Penetrative sex or exposure to bodily fluids, like semen, is not needed to contract HPV. It is transmittable by skin-to-skin contact during oral, vaginal, anal, and manual sex. It is most commonly transmitted from direct genital-to-genital contact (touching two sets of genitals together without a protective barrier). Some strains can be transmitted from kissing.
The CDC recently reported that HPV is contactable from mother to child through vaginal birth. Yet there is still much unknown about the virus. For example, the only studies released for HPV cases in children are from oral cancer cases. As the non-profit organization, HPV Awakening points out, no information has been released about whether or not children are being examined for anal, cervical or other cancers caused by HPV.
How is it diagnosed? HPV is detected from examination of warts and from tissue samples taken during a gynecological or urological exam. For women, a PAP smear does not test for the virus itself, but may detect precancerous condition that are caused by HPV. There are DNA tests that can be done with or without a PAP smear. These tests can determine if the type of HPV is a high-risk stain. For men, there is currently no FDA-approved HPV test, which means that men who have clear STI screenings with negative results should not consider themselves HPV-free or at zero-risk.
Is it curable or treatable? No. Warts can be removed. However, the virus may still remain in the body and can be transmitted to partners, and/or cause long-term health problems like cervical cancer.
Unfortunately, neither public awareness nor medical understanding of HPV matches these severely high statistics. Few people, both teens and adults, think about how a condom is only 70% effective against the virus or that a clear STI screening does not indicate that they are HPV-free. Blood banks do not screen for HPV.
And HPV is considered a “none-reportable” STI. This means that the US government and the CDC do not feel that individuals have a legal obligation to be informed by a partner that they have had a history of or currently have an “active” case of HPV.
Yet rather than acknowledging our unfamiliarity and unawareness of HPV we, the general public, continue to reinforce great social stigma with being diagnosed with an STI. And thus, the ignorance continues. This is precisely why the non-profit group HPV Awakening exists: to educate the general public and push for more investment in medical research.
 HPV Awakening Inc.: was founded by Tashia Ameneiro shortly after she was diagnosed with HPV at 25 years old. She contracted the virus from her first sexual partner who had known he was a carrier but did not tell her. It wasn’t long after that Tashia found herself trying to coop with a severe lack of public resources compounded with social stigma for being diagnosed with an STI. The impact of being diagnosed led her and her friends (Virginia Pena and Yvette Rodriguez) to launch HPV Awakening- A nonprofit to counteract social stigma through public education.
HPV Awakening Inc.: was founded by Tashia Ameneiro shortly after she was diagnosed with HPV at 25 years old. She contracted the virus from her first sexual partner who had known he was a carrier but did not tell her. It wasn’t long after that Tashia found herself trying to coop with a severe lack of public resources compounded with social stigma for being diagnosed with an STI. The impact of being diagnosed led her and her friends (Virginia Pena and Yvette Rodriguez) to launch HPV Awakening- A nonprofit to counteract social stigma through public education.
The Miami-based organization is the first established non-profit in North America to address general HPV that is not limited to one cancer form or another caused by HPV. They run workshops, lectures, and info booths at universities, schools and community events to raise public awareness about HPV and how to protect one self. They have partnered with major community-based organizations, such as the Village South/WestCare – Project IMPACT, hosting the First Cervical Cancer Day at FIU in January 2013 to provide a wide range of free health information to the public. HPV Awakening has also partnered with several student organizations such as VOX, WSSA (Women’s Studies Student Association), The Vagina Monologues, and One Billion Rising.
Along with improving public awareness, HPV Awakening is also putting pressure on the FDA and greater medical science community. They are pushing to make HPV caner strands “reportable” and get HPV male testing approved. They are also trying to expand medical and social research about the virus and the impact it has not only physically, but mentally and emotionally.
They need your support: As with all social causes, people’s support is essential to their survival. HPV Awakening functions through the hard work of just Tashia, her mother, and a few friends. They currently have no funding or sponsorship. All the things they have managed thus far have been done through their own pockets and free-time. They need support from everyone and have set up a donation bank on their website.
They desperately need funding for basic things like printing information pamphlets, free condoms to distribute, website management and sponsorship to attend relevant events like Gay Pride Fest- Miami Beach, AFO, and Exxxotica Expo.
They welcome any support. This includes actions as simple as sharing their facebook page or more involved help such as volunteering at their events and donating money to help them stay afloat.
HPV Awakening can be contact through through email @ Tashia@hpvawakening.org, phone 786 260 2092, and social media: facebook and twitter and experienceproject.
Here is an interview of HPV Awakening founder Tashia with NotiMujer
Found on http://hpvawakening.org/
Leave a Reply